 
Īssists in the diagnosis of left ventricular systolic dysfunction and valvular dysfunction. 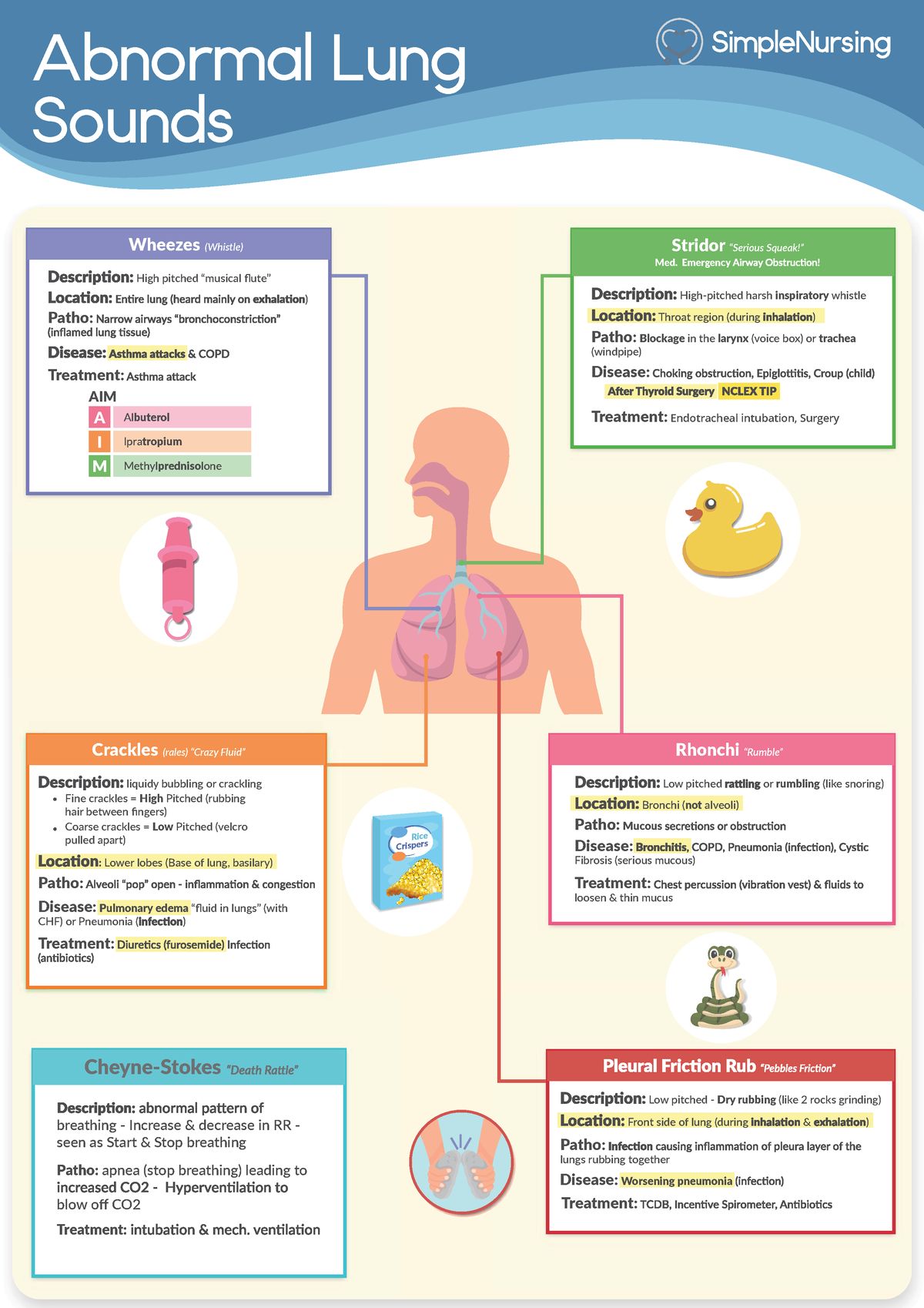
Pleural effusions are more commonly seen in the cardiogenic type. In noncardiogenic etiologies, the edema pattern is typically patchy and peripheral that can demonstrate the presence of ground-glass opacities and consolidations with air bronchograms. Cardiogenic pulmonary edema is characterized by the presence of central edema, pleural effusions, Kerley B septal lines, peribronchial cuffing, and enlarged heart size. Obtaining lipase and amylase levels help diagnose acute pancreatitis.īoth posteroanterior and lateral views in standard imaging or anteroposterior views in portable imaging are utilized. Obtaining serum electrolyte levels, including renal function, serum osmolarity, toxicology screening, help in patients with pulmonary edema due to toxic ingestion. 
Low albumin in isolation does not lead to pulmonary edema as there is a concurrent drop in pulmonary interstitial and plasma albumin levels preventing the creation of a transpulmonary oncotic pressure gradient. Hypoalbuminemia (≤3.4 g/dL) is an independent marker of increased in-hospital and post-discharge mortality for patients presenting in acute decompensated heart failure. They, however, are also noted to be elevated in patients with severe sepsis. Troponin elevation is commonly noted in patients with damage to myocytes, such as acute coronary syndrome. Levels between 100 and 500 pg/ml do not help in the diagnosis of heart failure and are often seen in critically ill patients. BNP levels less than 100 pg/ml suggest heart failure is less likely, and levels greater than 500 pg/ml suggest a high likelihood of heart failure. Elevated BNP levels correlate with left ventricular end-diastolic pressure as well as pulmonary occlusion pressure and can be seen in patients with congestive heart failure. It is a quick, inexpensive, and relatively less specialized test that can be done at the bedside.įollowing are a variety of diagnostic tools utilized to help diagnose pulmonary edema and, more importantly, differentiate between its different types.īrain-type natriuretic peptide (BNP) is secreted by the cardiac myocytes of the left ventricles in response to stretching caused by increased ventricular blood volume or increased intracardiac pressures. In addition to a thorough history and physical examination, electrocardiogram assists in diagnosing cardiac ischemia or myocardial infarction. 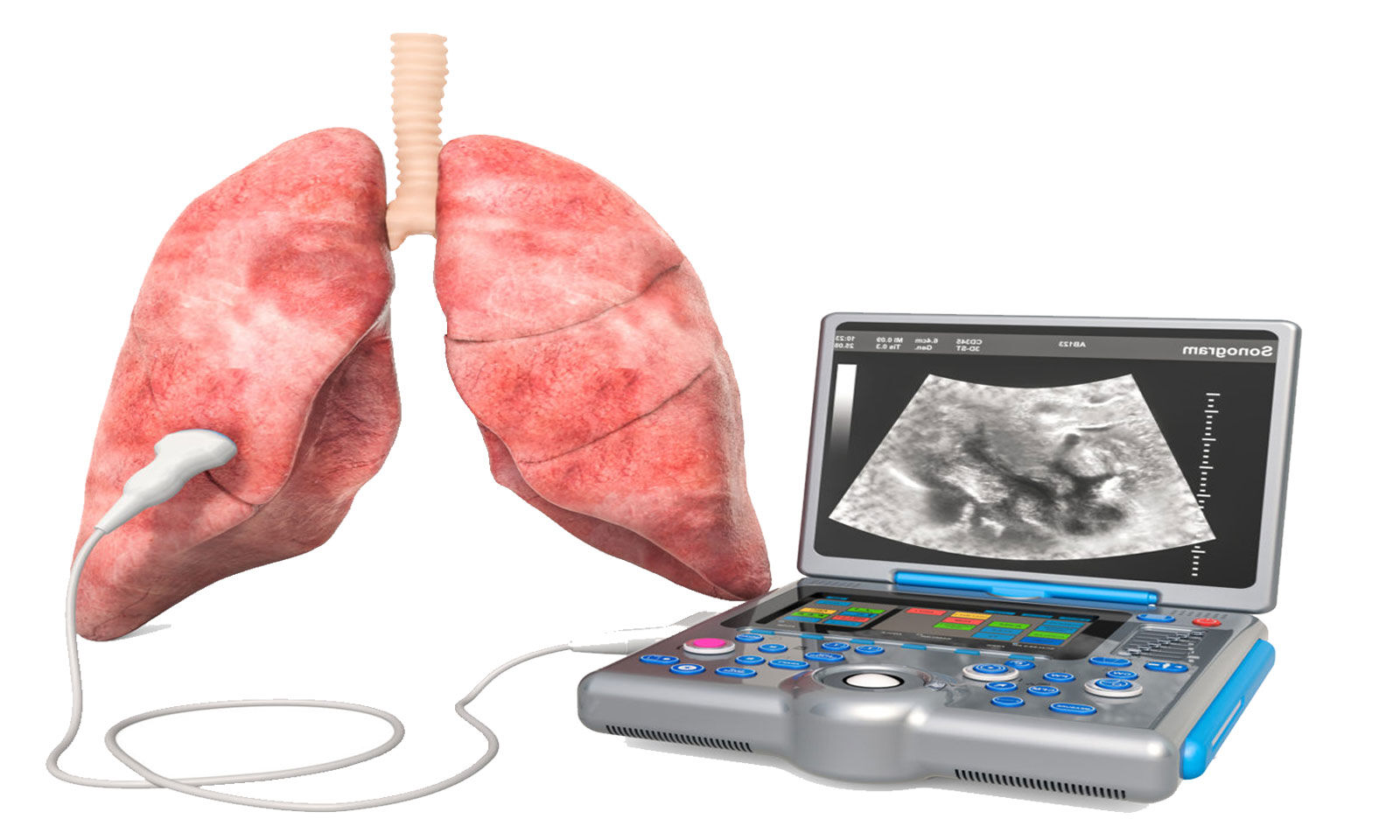
They are exclusively heard in the inspiratory phase when the small airways, which were shut during expiration, open abruptly. Fine crackles are heard in cardiogenic pulmonary edema. More specifically, hearing of either fine or coarse crackles is crucial to determine the next steps in the management. In patients with non-cardiogenic pulmonary edema, the symptoms of infections such as fever, cough with expectoration, dyspnea pointing to likely pneumonia, recent trauma, blood transfusions should be carefully assessed as these patients may progress to acute respiratory distress syndrome.Īuscultation remains the mainstay of bedside assessment in all patients with respiratory symptoms. Similarly, the presence of murmurs, elevated jugular venous pressure, peripheral edema may point towards a cardiac etiology. Progressively worsening dyspnea, tachypnea, and rales (or crackles) on examination with associated hypoxia are the clinical features common to both cardiogenic and noncardiogenic pulmonary edema.Ĭough with pink frothy sputum noted due to hypoxemia from alveolar flooding and auscultation of an S3 gallop could suggest cardiogenic edema. Acute lung injury with severe hypoxemia is referred to as acute respiratory distress syndrome (ARDS) and is seen in various conditions directly affecting the lungs, such as pneumonia, inhalational injury, or indirectly, such as sepsis, acute pancreatitis, severe trauma with shock, multiple blood transfusions. Noncardiogenic pulmonary edema is caused by lung injury with a resultant increase in pulmonary vascular permeability leading to the movement of fluid, rich in proteins, to the alveolar and interstitial compartments. This is typically seen in disorders involving left ventricular systolic and diastolic function (acute myocarditis including other etiologies of non-ischemic cardiomyopathy, acute myocardial infarction), valvular function (aortic/mitral regurgitation and stenosis in the moderate to the severe range), rhythm (atrial fibrillation with a rapid ventricular response, ventricular tachycardia, high degree, and third-degree heart block). Pulmonary edema can be broadly classified into cardiogenic and noncardiogenic pulmonary edema.Ĭardiogenic or volume-overload pulmonary edema arises due to a rapid elevation in the hydrostatic pressure of the pulmonary capillaries. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
